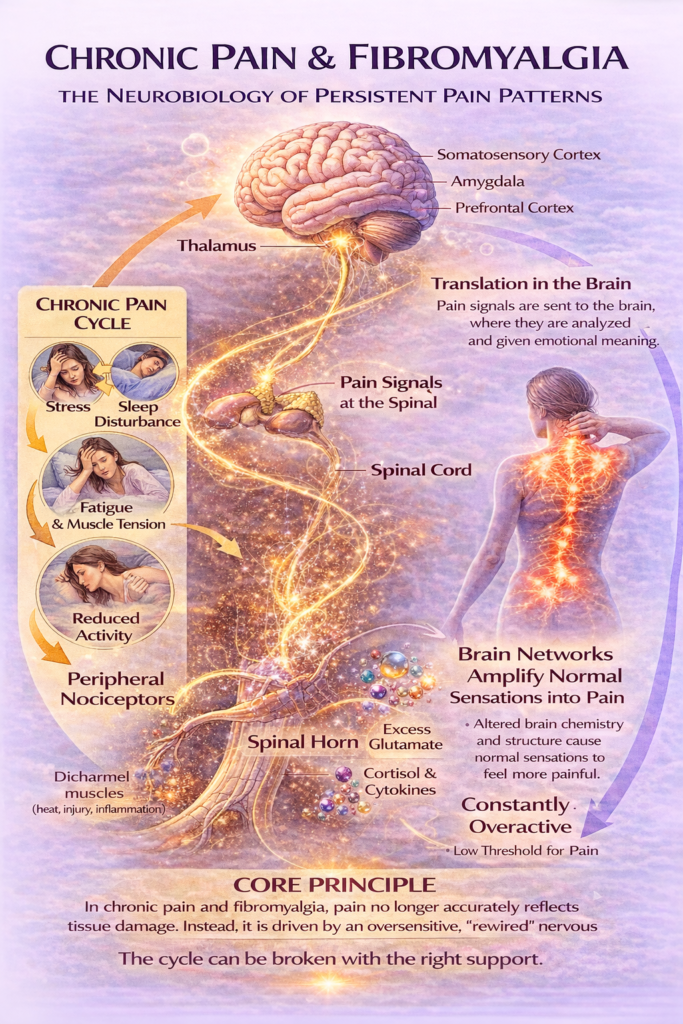
Chronic Pain and Fibromyalgia
Pain has traditionally been viewed as a direct indicator of tissue damage. Yet this simplified understanding reflects only the most basic level of physiological reality. In truth, pain is not generated in the muscles, joints, or connective tissues themselves. The sensation we experience as pain is constructed within the central nervous system, where sensory signals are integrated with emotional evaluation and cognitive interpretation. Through this complex process, a biological signal becomes a subjective experience of suffering.
In its acute form, pain serves an essential protective function. It warns the organism of potential harm, restricts further injury, and mobilizes the body’s resources for healing. But when pain becomes chronic, this protective mechanism loses its original purpose. Instead of reflecting ongoing tissue damage, it begins to operate autonomously, sustained by changes in neural regulation rather than by continued physical injury.
Modern neuroscience increasingly describes pain as a multilayered process. It begins with the activation of peripheral nociceptors—specialized receptors that respond to mechanical, thermal, or chemical stimulation. Yet this peripheral signal represents only the first stage in a much more complex chain of events. From the site of stimulation, the signal travels to the dorsal horn of the spinal cord, where it undergoes its first modulation. From there it reaches the thalamus and multiple regions of the brain, including the somatosensory cortex, the prefrontal cortex, and the amygdala.
The amygdala, in particular, plays an important role in assigning emotional significance to the signal. Under conditions of chronic stress—discussed in previous chapters—this emotional amplification can significantly intensify the subjective experience of pain.
It is at this point that the fundamental difference between acute and chronic pain becomes clear.
When pain follows an injury or inflammation, the nociceptive signal corresponds to actual tissue damage. In chronic pain, however, the central mechanism often becomes central sensitization. In this state, neural networks responsible for processing pain signals become increasingly excitable while losing some of their inhibitory control. The threshold for activation gradually decreases, while the intensity of the response increases. Stimuli that previously produced little or no discomfort may now be experienced as painful, even when the underlying tissues remain relatively healthy.
Fibromyalgia provides a clear clinical example of this phenomenon.
People with fibromyalgia experience widespread muscular pain, profound fatigue, sleep disturbances, and cognitive slowing. Yet laboratory tests typically show no signs of systemic inflammation or structural damage to the musculoskeletal system. For many years this absence of visible pathology led some clinicians to question the biological basis of the condition.
Today, however, advances in neuroimaging and neurochemical research have provided a clearer picture. Studies reveal increased activity in brain regions involved in pain processing, altered levels of neurotransmitters such as glutamate and serotonin, and reduced efficiency of descending inhibitory pathways that normally help regulate the flow of sensory signals.
Chronic stress appears to play a significant role in the development of this condition. Persistent activation of the amygdala and the HPA axis leads to elevated levels of cortisol and pro-inflammatory cytokines. These changes can influence pain thresholds and increase muscular tension. Muscles that remain in a state of constant micro-contraction begin to send signals of strain to the central nervous system. When those signals are processed within a sensitized neural network, they may be interpreted as persistent pain.
Over time, the nervous system consolidates this pattern. The pain signal becomes increasingly autonomous, no longer requiring a clear external trigger.
One characteristic feature of chronic pain is its shifting location. Patients often describe the pain as “moving” from one part of the body to another. This pattern suggests a central origin of the process. The primary dysregulation does not reside in a specific muscle or joint, but rather in the heightened neural processing of sensory input. In this state the nervous system becomes excessively vigilant, constantly scanning the body for potential signals of threat. Even minimal sensory input may be amplified, particularly when anxiety is present.
Behavioral adaptation also plays an important role in maintaining chronic pain. In an attempt to avoid worsening discomfort, individuals often begin to limit their movement. Although this response seems logical, prolonged reduction in physical activity can worsen the underlying condition. Reduced movement decreases microcirculation, lowers heart rate variability, and diminishes the production of endogenous opioids—the body’s natural pain-relieving substances.
Combined with increasing anxiety, this process gradually lowers the pain threshold even further. A self-reinforcing cycle emerges: pain restricts movement, and restricted movement intensifies pain.
A patient once described her experience in a way that captures this process vividly.
“My pain didn’t appear suddenly, and it wasn’t linked to a specific injury. It entered my life slowly. At first it was just tension in my neck after a long day at work. Then stiffness appeared in my lower back. Later I began to feel a heavy, spreading pressure in my shoulders and legs, as if my body were carrying an invisible weight.
I went through medical examinations, did blood tests, followed the recommendations of specialists—but everything was ‘within normal limits.’ Eventually I began doubting my own experience, because I had no objective proof of suffering.
The pain had no fixed location. It could disappear from one place and appear in another. Sometimes it intensified without any clear reason; sometimes it faded briefly, creating the illusion of improvement.
I began to fear movement, because every unfamiliar effort seemed like a risk of making the pain worse. But the more careful I became, the more fragile and restricted my body began to feel.
At some point I stopped asking why the pain existed. Instead, I started planning my days around the assumption that it would be there. That expectation slowly became part of my identity.
I had lived with the pain for so long that the idea of life without it began to feel almost unrealistic.”
This example illustrates the development of a stable neural pattern in which central nervous system sensitization is sustained by both biological and behavioral factors.
Sleep disturbance plays a particularly important role in maintaining chronic pain. During deep sleep the brain regulates neurotransmitter balance and restores receptor sensitivity. Research shows that even short-term reductions in slow-wave sleep can increase pain sensitivity the following day.
This creates another reinforcing cycle: pain disrupts sleep, and insufficient sleep amplifies pain.
Despite the complexity of these mechanisms, it is crucial to emphasize that many of them remain reversible, especially when structural tissue damage is absent. Neuroplasticity—the same property that allows the nervous system to form persistent pain patterns—also allows it to relearn healthier patterns of regulation.
Gradual restoration of sleep quality, reduction of chronic stress activation, and carefully graded physical activity can help retrain the nervous system. Movement must be introduced progressively, not in a way that intensifies sensitization but in a way that teaches the nervous system that the body can move safely again.
Through this process, the individual gradually regains a sense of control over their own body.
Chronic pain and fibromyalgia, in many cases, are not inevitable consequences of tissue destruction. They represent a sustained change in the way the central nervous system processes sensory information. Understanding this neurobiological foundation allows a person to move away from passive acceptance of suffering toward an active and structured strategy of recovery.
CORE PRINCIPLE OF THE CHAPTER:
Chronic pain in the absence of structural damage often results from persistent central sensitization and altered neural regulation. Because these processes involve adaptive neural plasticity, they may gradually be reversed through systemic restoration of physiological balance.
Written by Alexander Babinets
Founder of Express Fitness, certified coach, and author helping people get in shape without excuses.
THIS IS A CHAPTER FROM MY NEW BOOK: 12 STEPS TO FREEDOM: Conquering DEPRESSION and Taking Back Your Life
📍 expressfitness.ca | 📩 info@expressfitness.ca
👤 More about me → alexanderbabinets.com
