Neurophysiology of Anxiety
In the previous chapters we examined compensation and chronic stress as biological processes. Now we need to move one level deeper—to the place where the sense of danger is actually generated, even when no objective threat exists. This level involves the activity of the amygdala, a small but powerful structure in the brain, and its interaction with the autonomic nervous system, particularly the vagus nerve.
Anxiety does not arise out of nowhere. It has a clear neurophysiological architecture.
The Amygdala as the Brain’s Threat Detector
The amygdala is a small structure located deep within the temporal lobes of the brain. It plays a central role in emotional processing, especially in the rapid detection of potential threats.
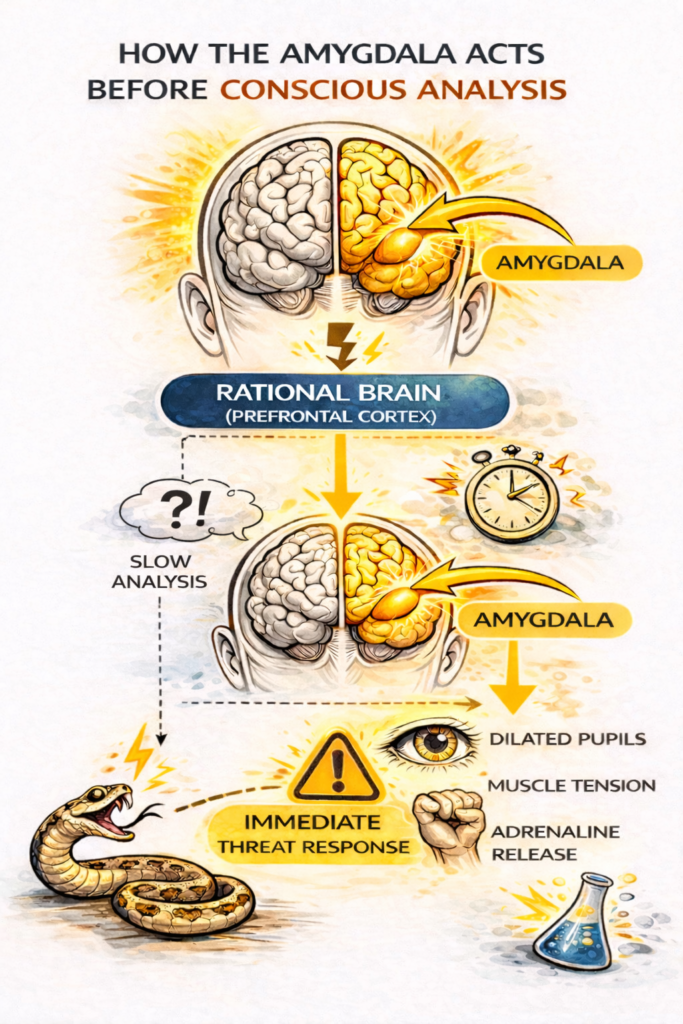
One important feature of the amygdala is that it responds faster than the prefrontal cortex, the part of the brain responsible for rational analysis and conscious decision-making. Signals related to possible danger can travel along a “short pathway,” moving directly from sensory centers to the amygdala before the thinking brain has time to evaluate the situation.
This is why people often feel a surge of fear or anxiety before they have time to logically assess what is happening.
From an evolutionary perspective, this system makes sense. In a dangerous environment, a delayed response could mean death. Reacting to a harmless stimulus is far less dangerous than ignoring a real threat.
But in the modern world, this ancient survival mechanism can become overactive.
Imagined Threats, Real Reactions
For the amygdala, there is not always a clear distinction between physical danger and vividly imagined scenarios. If a thought is interpreted as a threat, the biological stress response can be activated.
Heart rate increases.
Muscle tension rises.
The HPA axis becomes active.
Parasympathetic regulation decreases.
All of this can happen in complete silence, in a bedroom at night, without any external stimulus.
When this cycle repeats over time, neural pathways become reinforced. The amygdala becomes more sensitive to potential signals of danger, and the threshold for its activation gradually lowers. What develops is hyperreactivity.
Anticipatory Anxiety
One of the most subtle and persistent forms of amygdala activity is anticipatory anxiety. In this state, a person does not fear an event itself, but the possibility that the event might happen again.
This pattern is especially visible in sleep disturbances.
A single night of poor sleep does not harm the body. However, the thought “What if I can’t sleep again tonight?” can activate the brain’s threat system long before bedtime arrives.
Heart rate increases.
Cortisol levels rise.
Muscle tension remains elevated.
The body prepares for danger at the very moment when it should be preparing for restoration. Over time, this creates a downward spiral.
The Vagus Nerve as a Counterbalance
The vagus nerve is one of the most important channels of parasympathetic regulation. High vagal activity is associated with states of safety, recovery, and social connection.
When the amygdala becomes highly active, parasympathetic tone tends to decrease. Conversely, when parasympathetic activity increases, the reactivity of the amygdala often diminishes.
This relationship works in both directions.
For this reason, effective regulation of anxiety cannot occur without restoring balance within the autonomic nervous system.
The Plasticity of Fear
The brain is highly adaptable. When certain thoughts repeatedly trigger anxiety responses, the neural circuits associated with those reactions become stronger.
Over time, activation becomes automatic. A person may no longer even recognize the thought that originally triggered the response. All that remains is a persistent sense of inner tension.
Eventually people may say, “That’s just the way I am,” without realizing that anxiety has become a learned pattern within the nervous system.
A patient once described his experience in a way that illustrates this process clearly.
“It started gradually. I had never considered myself an anxious person. But after a period of intense pressure at work, I began noticing strange episodes.
I would lie in bed at night, everything quiet, and suddenly a thought would appear: What if my heart stops? And the moment that thought appeared, my heart would begin beating harder.
I knew the idea was irrational, yet the sensation felt completely real.
I tried to reassure myself that everything was fine, but my body was no longer listening. Heat would rise through my chest, my breathing became shallow, and tension spread through my muscles.
Eventually the episode passed.
The next evening, however, I went to bed already expecting it to happen again—and it did.
After a month I began to fear the evenings themselves. During the day I functioned normally. I worked, smiled, fulfilled my responsibilities. But inside there was a constant alarm signal that seemed to have no clear cause.
Medical examinations revealed nothing unusual. I was told it was ‘just nerves.’
But it didn’t feel like ordinary worry. It felt as if my own brain was manufacturing a threat even when none existed.”
This example illustrates the amygdala operating in a state of hypersensitivity. No external event is necessary. The internal scenario is enough.
The Role of Sleep in Amygdala Regulation
Research shows that chronic sleep deprivation increases the reactivity of the amygdala while weakening the regulatory influence of the prefrontal cortex.
In other words, insufficient sleep makes the brain more sensitive to perceived threats. Each night of poor sleep increases the likelihood that neutral situations will be interpreted as dangerous.
A self-reinforcing cycle emerges:
sleep deprivation → increased emotional reactivity → anxious thoughts → further sleep disruption.
Cognitive Reinforcement
When anxious thoughts repeat frequently, a stable cognitive pattern begins to form. Neutral signals are interpreted as potential threats. This is not a sign of weak character. It is the result of neural learning.
And like any learned pattern, it can also be reshaped.
Practices That Support Regulation
Activation of the vagus nerve can occur through several physiological pathways, including slow breathing, extended exhalation, meaningful social interaction, moderate physical movement, and the deliberate cultivation of gratitude.
The last of these is sometimes dismissed as a purely psychological recommendation. In reality, it also has a physiological basis. When attention is intentionally directed toward positive aspects of experience, the reactivity of the amygdala decreases while prefrontal regulatory circuits become more active.
This is not a form of mental magic. It is a demonstration of neuroplasticity.
From Anxiety to Stability
The goal of regulation is not the suppression of emotion. The goal is restoring balance between neural systems.
When the amygdala is no longer chronically hyperreactive and parasympathetic tone returns, a sense of internal safety begins to reappear. At that point people often describe a profound shift: they no longer feel as though their own brain is working against them.
CORE PRINCIPLE OF THE CHAPTER:
The amygdala responds not to reality itself, but to the brain’s interpretation of it. When chronically activated, it can sustain a sense of threat even in conditions of objective safety.
Written by Alexander Babinets
Founder of Express Fitness, certified coach, and author helping people get in shape without excuses.
📍 expressfitness.ca | 📩 info@expressfitness.ca
👤 More about me → alexanderbabinets.com
THIS IS CHAPTER FROM MY NEW BOOK. READ MORE HERE: 12 STEPS TO FREEDOM: Conquering DEPRESSION and Taking Back Your Life
